User:Mr. Ibrahem/Myelodysplastic syndrome
| Myelodysplastic syndrome | |
|---|---|
| Other names | Preleukemia, myelodysplasia[1][2] |
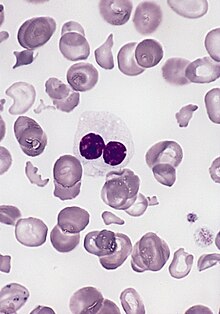 | |
| Blood smear from a person with myelodysplastic syndrome. A hypogranular neutrophil with a pseudo-Pelger-Huet nucleus is shown. There are also abnormally shaped red blood cells, in part related to removal of the spleen. | |
| Specialty | Haematology, oncology |
| Symptoms | None, feeling tired, shortness of breath, easy bleeding, frequent infections[3] |
| Usual onset | ~ 70 years old[4] |
| Risk factors | Previous chemotherapy, radiation therapy, certain chemicals such as tobacco smoke, pesticides, and benzene, exposure to mercury or lead[3] |
| Diagnostic method | Blood test, bone marrow biopsy[3] |
| Treatment | Supportive care, medications, stem cell transplantation[3] |
| Medication | Lenalidomide, antithymocyte globulin, azacitidine[3] |
| Prognosis | Typical survival time 2.5 years[3] |
Myelodysplastic syndromes (MDS) are a group of cancers in which immature blood cells in the bone marrow do not mature, so do not become healthy blood cells.[3] Early on, no symptoms typically are seen.[3] Later, symptoms may include feeling tired, shortness of breath, easy bleeding, or frequent infections.[3] Some types may develop into acute myeloid leukemia.[3]
Risk factors include previous chemotherapy or radiation therapy, exposure to certain chemicals such as tobacco smoke, pesticides, and benzene, and exposure to heavy metals such as mercury or lead.[3] Problems with blood cell formation result in some combination of low red blood cell, platelet, and white blood cell counts.[3] Some types have an increase in immature blood cells, called blasts, in the bone marrow or blood.[3] The types of MDS are based on specific changes in the blood cells and bone marrow.[3]
Treatments may include supportive care, drug therapy, and stem cell transplantation.[3] Supportive care may include blood transfusions, medications to increase the making of red blood cells, and antibiotics.[3] Drug therapy may include the medications lenalidomide, antithymocyte globulin, and azacitidine.[3] Certain people can be cured with chemotherapy followed by a stem-cell transplant from a donor.[3]
About seven per 100,000 people are affected with about four per 100,000 people newly acquiring the condition each year.[4] The typical age of onset is 70 years.[4] The outlook depends on the type of cells affected, the number of blasts in the bone marrow or blood, and the changes present in the chromosomes of the affected cells.[3] The typical survival time following diagnosis is 2.5 years.[4] The conditions were first recognized in the early 1900s.[5] The current name came into use in 1976.[5]
References[edit]
- ^ "Myelodysplasia". SEER. Archived from the original on 27 October 2016. Retrieved 27 October 2016.
- ^ "Myelodysplastic Syndromes". NORD (National Organization for Rare Disorders). Archived from the original on 4 December 2019. Retrieved 23 May 2019.
- ^ a b c d e f g h i j k l m n o p q r s "Myelodysplastic Syndromes Treatment (PDQ®)–Patient Version". NCI. 12 August 2015. Archived from the original on 5 October 2016. Retrieved 27 October 2016.
- ^ a b c d Germing, U; Kobbe, G; Haas, R; Gattermann, N (15 November 2013). "Myelodysplastic syndromes: diagnosis, prognosis, and treatment". Deutsches Ärzteblatt International. 110 (46): 783–90. doi:10.3238/arztebl.2013.0783. PMC 3855821. PMID 24300826.
- ^ a b Hong, Waun Ki; Holland, James F. (2010). Holland-Frei Cancer Medicine 8 (8 ed.). PMPH-USA. p. 1544. ISBN 9781607950141. Archived from the original on 2016-10-27.
